
#Weekend Music Share




Your Friday prompt for Stream of Consciousness Saturday is start your post with a preposition.
The heat is oppressive outside, I open the door to let Griffy in and a wave of heat knocks me backwards. In Texas it’s been at or over 100 for weeks now and it’s wearing on me, that says a lot because I’m a native Texan. I count the days until September when cooler days will replace the heat. M
Here are the rules for SoCS:


1851
The ‘Auld Mug’ trophy is awarded for the first time to the winners of a sailing race around England’s Isle of Wight. The schooner ‘America’ sails into first place with an ample lead, and so the competition between the world’s best racing yachts will be known as the ‘America’s Cup.’
1902
Named for the man who founded Detroit in 1801, Antoine Laumet de La Mothe Cadillac, Michigan’s newest car company launches. The Cadillac Automobile Company rises from the ashes of the Henry Ford Company, after Ford leaves his company over a squabble with investors.
1986
Rob Reiner’s ‘Stand by Me’ hits theaters. Based on Stephen King‘s novella ‘The Body,’ the movie tells the story of four boys searching for a missing boy’s corpse. ‘Stand by Me’ will help make stars out of Wil Wheaton, River Phoenix, Corey Feldman, and Jerry O’Connell, and earn more than $52 million at the box office.
BIRTHDAYS
James Corden, 40 Comedian
Valerie Harper, 80 Actress
Cindy Williams, 72 Actress
The sheet touches the underside of my arm and it burns.
My sandals touch a spot on my foot that shoots pain up my leg.
Sleeping is restless since shoulder and hip joints have painful arthritis.
Motivation for anything is non existent.
Sleeping requires narcotics, I hate the way they make me feel the next day.
Walking the day in a brain fog.
Keep changing crossed legs because of pain in each leg.
Depression creeps in and there’s no way to close the trap.
I work to keep hopes high during the day but realize at some point pain has overcome my body.
I pray tomorrow is a better day.
M
By David Konow 08/06/19
Bell revealed on Instagram that lately she’s been “feeling very off,” but she is utilizing resources and her support system to help her through it.

Kristen Bell, star of Veronica Mars, is one of many celebrities who has been open about her mental health. She recently posted on her Instagram story, “Lately I’ve been feeling very off.”
Bell added, “I’m checking in with my support systems and my resources and I hope you are too because we can handle whatever life throws at us if we ask for hope.”
Several days earlier, Bell posted a picture of herself in a split image. In one image, she looked happy, in another image, she looked depressed. “Ever feel like this?” she wrote. “Me too. Often. It’s okay to not feel ok. We’ll get through it together.”
On Instagram, Bell also suggested ways to battle back against tough mental health days, like going on Google and looking up “workouts near me, mental health resources near me, therapists near me, support groups near me.”
In previous interviews, Bell has been very open about her mental health struggles. She learned about her family’s difficulties with mental health when she was 18. Her mother told her that there was “a serotonin imbalance in our family line, and it can often be passed from female to female.” Her grandmother had endured electroshock therapy, and Bell learned how to take care of her own mental health through her mother.
When Bell decided to go on medication, her mother told her “the world wants to shame you for that. But in the medical community, you would never deny a diabetic his insulin. But for some reason, if someone needs a serotonin inhibitor, they’re immediately crazy or something.”
Last year, Bell participated in a campaign for the Child Mind Institute, where she posted a message to her younger self, saying, “People seem like they don’t have problems, but everyone’s human. Everyone has problems. Everyone feels yucky on the inside sometimes. I have suffered from anxiety and/or depression since I was 18. What I would say to my younger self is don’t be fooled by this game of perfection that humans play. Because Instagram and magazines and TV shows, they strive for a certain aesthetic, everything looks so beautiful, and people seem like they don’t have problems, but everyone’s human.”
In addition to contributing for The Fix, David Konow has also written for Esquire, Deadline, LA Weekly, Village Voice, The Wrap, and many other publications and websites. He is also the author of the three decade history of heavy metal, Bang Your Head (Three Rivers Press), and the horror film history Reel Terror (St Martins Press). Find David on LinkedIn and Facebook.

Ingredients
8 tablespoons (1/2 cup) butter or nondairy alternative (Earth Balance Buttery Sticks)
8 tablespoons (1/2 cup) shortening (or Earth Balance Shortening Stick)
1 cup firmly packed light brown sugar
1/2 cup granulated cane sugar
3/4 teaspoon sea salt
2 teaspoons gluten-free vanilla extract (Neilson Massey Madagasgar Bourbon Vanilla)
2 large eggs (or reconstituted Ener-G egg replacer or applesauce)
1 teaspoon baking soda
1/2 teaspoon baking powder
2 1/2 cups Jules Gluten-Free All Purpose Flour or other brand
12 ounces semisweet chocolate chips or dairy-free chocolate chips, peanut butter chips, white chocolate chips (available dairy-free), M&M’s, or a mixture
Bring the butter and shortening to room temperature and then beat together with sugars until light and fluffy (several minutes). Mix in the vanilla extract and eggs until combined.
In another bowl, whisk together dry ingredients. Gradually stir these dry ingredients into the sugar mixture. Stir in chips and nuts, if so desired.
Scoop dough into a container (metal, if possible) and cover tightly. Refrigerate of freeze until very cold (overnight is ideal). Preheat oven to 350 degrees (static) or 325 degrees (convection).
Drop measured tablespoons onto cookie sheet lined with parchment paper, at least 1 inch apart. Bake 8-9 minutes, or until the tops are lightly browned. Let them stand 5 minutes before removing them from cooling racks.
Makes approximately 60 cookies






Have a great weekend, stay safe and hydrated. M



| We are almost to our goal! Thank you so much to this amazing community for your support! We have raised over 80% of the funds to access this amazing database that will help us fund the future of Lyme disease! We are only $760 short!For the past 3 years, Lyme Warrior has been working to fund research & patient care through grassroots fundraising and it is time for us to give the community significantly more of the support and it needs and deserves. _____ This program will allow access to a research and development database that will open doors for us to:•Fund more & signing larger research programs •Fund a patient care program to help offset medical costs for Lyme patients •Start a housing community for Lyme patients in need _____Please visit http://lymewarrior.us/open-doors to see how YOU can help us make change happen! Any amount truly helps! 💚💚💚 ThaLearn MoreAs a small token of our gratitude, donations over $50 will receive a custom made Opening Doors keychain from us for helping us make big change for our community.Thank you for your amazing support! |
| Copyright © 2019 Lyme Warrior US, All rights reserved. You subscribed to LW mailing list. Our mailing address is: Lyme Warrior US228 Givens Branch TrailNewport, Va 24128 |

Have a great Woodstock kind of day! I can’t believe I was only seven years old. Stay hydrated. M
1483
Pope Sixtus IV consecrates a chapel in Rome after painters, including Botticelli, have finished their frescos. The ceiling, however, still needs a little work, and 25 years later a new pope will hire Michelangelo to paint what will be considered one of the greatest artworks of all time.
1914
Thirty-three years of toil comes to a close as one of the greatest engineering achievements in human history, a 51-mile-long channel carved through the Isthmus of Panama, opens to maritime traffic. The new shortcut between the Pacific and Atlantic will speed transport and remake the global economy.
1947
British Crown Rule ends in one of the most populous places on the planet, the vast, diverse country of India. Although the Dutch, Danish, and French were there before them, Britain has had a presence on the vast subcontinent since 1612. Today, however, India gains its freedom.
1969
Max Yasgur’s farm fills with masses of music lovers as the Woodstock Music and Art Fair kicks off its first day. Before the event is through, 400,000 will revel in rainstorms and mud, some of history’s best rock bands will jam, and a counterculture will consider itself transformed.


It’s important to understand what glutens are and where to look for in order to establish a gluten-free lifestyle. As more people are diagnosed gluten intolerant more pre-made products will become available making choices much easier. I plan to write a number of post on the Gluten-Free lifestyle in the coming months. Below is a short list of items and ingredients you can eat. The Information is taken from Gluten Freedom by Alessio Fasano, MD. Founder and Director of the Center for Celiac Research at Massachusetts General Hospital Harvard Medical School. Melinda
Gluten is found in common foods such as breads, cereals, baked goods, and pasta. Because it’s used in processed foods as an additive or preservative, gluten is also found in a wide variety of foods and nonfood items from prescription medications to Play-Doh. If you are the food shopper in the family, you must learn to read labels very carefully to comply with gluten-free diet.
Things you can eat on the Gluten-Free Diet
Gluten-Free Grains, Flours, Seeds and Starches
Safe Ingredients List
Melinda

Your Friday prompt for Stream of Consciousness Saturday is “where.” Start your post with the word “where” and write whatever comes to you. Bonus points if you end your post with “where” too. Enjoy!
Where is this post going? I don’t know yet but have read some good ones this morning starting with “where”. Where does my dog get the idea I’m a snack machine, every action he makes he thinks is worthy of a snack. We don’t have children so we do spoil both of our dogs rotten, and they know it. I have to wipe my older dogs chin off after eating and clean his face, he thinks it deserves a snack.
Where is my snack, well my treat came this early a.m. in the form of a Starbucks Grande Latte and a blueberry muffin delivered right to my beside. Maybe I’m a little spoiled too. That’s our weekend ritual, my husband gets breakfast and me a coffee, we eat and then take a nap. What a wonderful way to spend a Saturday and Sunday morning.
This post was going where?


Here are the rules for SoCS:

Psychology Today
Posted Jul 29, 2019
What is your sense of stillness?
“Stillness or peace” may sound merely sentimental (“visualize whirled peas”). But deep down, it’s what most of us long for. Consider the proverb: The highest happiness is stillness.
Not a stillness or peace inside that ignores a pain in oneself or others or is acquired by shutting down. This is a durable stillness, a stillness you can come home to even if it’s been covered over by fear, frustration, or heartache.
When you’re at peace–when you are engaged with life while also feeling relatively relaxed, calm, and safe–you are protected from stress, your immune system grows stronger, and you become more resilient. Your outlook brightens, and you see more opportunities. In relationships, feeling at peace prevents overreactions, increases the odds of being treated well by others, and supports you in being clear and direct when you need to be.
How?
I think there are different kinds of stillness, and I’ll point out where each might be found. The first two kinds are pretty straightforward, while the third and fourth take a person into the deep end of the pool. It’s helped me to notice, appreciate, and (hopefully) practice each of these. It’s okay to focus on just one for a while; any peace is better than none!
In particular, enjoy your stillness, wherever you find it. In our culture of pressure, invasive demands for attention, and jostling busyness, inner peace must be protected. When you experience it, enjoy it, which will help it sink into you, weaving its way into your brain so it increasingly becomes the habit of your mind.
The Stillness of Ease
This is the stillness of relaxation and relief, and it comes in many forms. You look out a window and feel calmer, talk through a problem with a friend, or finally make it to the bathroom. You exhale slowly, activating the soothing parasympathetic wing of your nervous system. You finish a batch of emails or dishes. You were worried about something but finally, get good news.
Whew. At rest. It’s easy to underestimate this sort of stillness or peace but it really counts. Take it in when you feel it.
The Stillness of Tranquility
This is deep quiet in mind and body. Perhaps you’ve felt this on first waking before the mind kicks into gear. Or while sitting next to a mountain pond, something of its peace seeps into your heart. At the end of a workout, meditation, or yoga, you might have felt serene.
When mind and body are this settled, there is no sense of deficit or disturbance, and no struggling with anything, or grasping after it, or clinging to others. There’s inner freedom, a non-reactivity, that is wonderful.
The Stillness of Awareness
This is a subtler kind of stillness. Perhaps you’ve had the experience of being upset and your mind is racing . . . and at the same time, there is a place inside that is simply witnessing, untroubled by what it sees. Or you may have the sense of awareness as an open space in which sights and sounds, thoughts and feelings, arise and disappear; space itself is never ruffled or harmed by what passes through it.
I’m not speaking of anything mystical here, only what you can see directly in your own mind. As either a bare witness or space through which the stream of consciousness flows, awareness itself is always still.
The Stillness of What’s Unchanging
First, while most things continually change, some don’t; for example, the fact that things change doesn’t itself change. Two plus two will always equal four. The good thing you did this morning or last year will always have happened. Things that don’t change are reliable, which feels the stillness.
Second, while individual waves come and go, the ocean is always the ocean. While the contents of the universe are changing, the universe as the universe is not. You can get an intuition of this by recognizing that you are a local wave in a vast sea of human culture, nature, and the physical universe; yes, you are changing, but within an unchanging allness. The sense of this, even if fleeting, can really put you at peace.
Third, you could have a sense of something transcendental, something eternal, call it God, Spirit, the Unconditioned, or by no name at all. Beyond words, this offers “the peace that passeth understanding,” and I include it here because it is meaningful to many people (including myself).
* * *
May we all find stillness.
Like this article? Receive more like it each week when you sign up for Rick Hanson’s free Just One Thing Newsletter.




Thank you for stopping by today, I enjoy your comments. Have a great weekend. M
| Good Day, The August series of my Lyme Q&A Webinar begins this Thursday. I have three webinars planned on Thursdays. Did you sign up? Join my Lyme Q&A Webinar, Conversations with Marty Ross MD, to get answers. If you read this before Thursday 6 PM CST, it is not too late. Each week is NEW. No two Lyme Q&A Webinars are the same because you create each one with your questions. What do you want to know about Lyme? I have an answer for that! Find ways to improve your Lyme disease treatment. I am ready to help your recovery. Join me for the next Conversations with Marty Ross MD. Sign up now to reserve your space for this Thursday. Ask your Lyme disease questions in my live webinar called Conversations with Marty Ross MD. In this webinar you willlearn fresh ideas to take back your health and life. No two webinars are alike because they are designed by your questions. Join me in my mission to improve lives. Please forward this email to anyone you know who has Lyme disease who will benefit from one of my Lyme Q&A Webinars. So what are you waiting for? Sign up now to reserve your space for Thursday at 6 PM CST. I look forward to helping you. In Health, Marty Ross MD, LLMD Sign Up! |
July 23, 2019/ U.S. Pain Foundation
Too often, due to broad misconceptions and a lack of understanding about pain, pain warriors are afraid or ashamed to speak up about their stories.
But the only way we can create change is if we start talking–to loved ones, coworkers, neighbors, clinicians, and even policymakers.
That’s why our theme for Pain Awareness Month 2019, which begins September 1, is “Let’s Talk about Pain.” We’ll be hosting numerous events, campaigns, and activities that center around this idea. In order to truly get the word out, though, we need your help.
Below, please find a short list of ways you can participate right now in Pain Awareness Month. Many of these campaigns require involvement before September, so don’t wait!

Submit your video story! Share a 3-5 minute video about your pain journey with us by August 9. All participants will receive a limited-edition Pain Awareness Month bracelet and our new Living with Pain educational booklet–AND be entered to win a prize pack. A handful of individuals will be selected to have their videos featured online throughout September! Get started here. Questions? Email us.

Request a proclamation. Ceremonial proclamations from state and local representatives help bring awareness to pain at the government level. To get started, fill out this form by August 9. We have easy-to-use templates and tips to make the process easy and fun. Please note that proclamations can take time, so put in your request now! For questions, email us.

Host an information table. Hosting an information table at a local hospital, library, town hall, or even a retail store is a great way to educate your community about pain. We’ll provide all the materials you need, including table cloths, brochures, and giveaway items. Simply fill out the questionnaire here. Keep in mind we need two weeks’ notice to ship materials!

Shine Blue for Pain. Through this campaign, you can request a government, historic, or private building or landmark light up in blue–the designated color for pain–on September 13. To get involved, fill out this form or send us an email by August 15. We’ll give you all the tools you need to make your request. Be sure to take a photo so we can celebrate your hard work!

Organize a Wear Blue Day. New this year, we’re encouraging people with pain to host Wear Blue Days at their schools or workplaces! By rallying together and wearing the designated color for pain, people with pain can feel included and supported. And, it helps raise awareness about the issue of pain on a large scale. For information on how to get involved, send us an email.

Help Beautify in Blue. Through this visual campaign, volunteers display blue ribbons and flyers in public locations such as town halls, community centers, libraries, municipal parks, or grassy areas. We provide a template letter to request permission to display the materials, as well as the materials you need (at no cost to you). Get started here.
To learn more about all Pain Awareness Month 2019 activities, visit our website. And remember to keep an eye out for more details about our social media challenge and weekly events.
If you have any questions about getting involved, please email us at painawareness@uspainfoundation.org.GET INVOLVED NOW!

Surveillance case definitions are not intended to be used by healthcare providers for making a clinical diagnosis or determining how to meet an individual patient’s health needs – CDC
The Centers for Disease Control and Prevention (CDC) has agreed to add a disclaimer to the surveillance case definition for Lyme disease that it is “not intended to be used by healthcare providers for making a clinical diagnosis or determining how to meet an individual patient’s health needs.”
According to a July 16 letter from Lyle Peterson, MD, Director of the CDC Division of Vector-Borne Diseases, this change is being implemented on “all individual case definition pages, including the 2017 Lyme disease case definition page.”
This action was taken following an Information Quality Request for Correction complaint filed by the Patient Centered Care Advocacy Group on May 20, 2019.
According to the complaint, many healthcare providers incorrectly rely on the case definition to interpret results of the two-tier test, resulting in large numbers of patients who are misdiagnosed and denied medically necessary treatment and insurance coverage. This situation worsens the Lyme epidemic and increases the financial impact on our country in terms of lost productivity, disability, and increased medical expenses.
The CDC disclaimer states:
“A surveillance case definition is a set of uniform criteria used to define a disease for public health surveillance. Surveillance case definitions enable public health officials to classify and count cases consistently across reporting jurisdictions. Surveillance case definitions are not intended to be used by healthcare providers for making a clinical diagnosis or determining how to meet an individual patient’s health needs.”
According to the case definition for Lyme disease, most patients must either have an erythema migrans rash (EM, also known as a bull’s eye rash) or test positive on a two-tier blood test according to a narrow threshold. Yet many patients never get a rash, and a systematic meta-analysis of published data shows the mean sensitivity of two-tier test to be only 35.4% in the acute stage and 64.5% in the convalescent stage, with an overall sensitivity of 59.5%. The unreliability of the two-tier test is compounded by widespread misconception by healthcare providers and insurers that patients must test positive according to the surveillance criteria to confirm they have a legitimate case of Lyme disease.
“The disclaimer is a step in the right direction,” said Bruce Fries, President of the Patient Centered Care Advocacy Group, “but a lot more needs to be done to educate healthcare providers that the two-tier test is unreliable and the case definition should not be used for diagnosis. CDC has been encouraged by Congress as far back as 2002 to aggressively pursue and correct the misuse of the definition. Unfortunately, however, little was done and the case definition continues to be misused.”
Following are links to the complaint and CDC’s response.
Information Quality Request for Correction
www.lymepatientadvocacy.org/Documents/CDCInfoRequestforCorrection-05-20-2019.pdf
CDC Response
www.lymepatientadvocacy.org/Documents/CDCResponse-071619-CaseDefinition.pdf
TED TALKS
Jul 22, 2019 / Daryl Chen

Justin Tran
This post is part of TED’s “How to Be a Better Human” series, each of which contains a piece of helpful advice from someone in the TED community; browse through all the posts here.
“Doctor, is this really necessary?”
Oslo neurosurgeon Christer Mjåset, vice president of the Norwegian Medical Association, says that he experienced a jolt when a woman asked him this question, he recalls in a TEDxOslo talk. It was a first in his career — he’d never had a patient say this to him.
It occurred after Mjåset suggested spinal surgery to her; she was troubled by intense pain caused by a herniated cervical disc. While he’d performed this procedure many times before, it did come with risks — with paralysis from the neck down being one of the most serious. This led the patient to ask: “Doctor, is this really necessary?”
“You know what I realized right there and then?” Mjåset says. “It was not.”
When he looked more deeply at his motives, he saw that he’d been largely driven by enthusiasm for his work. He says, “I have to admit: I wanted to operate. I love to operate. Operating is, after all, the most fun part of my job.”
There’s a stark imbalance in the healthcare system in much of the world — while medical treatment is extremely difficult and expensive for some to access, it’s overly easy for others. Thanks to this patient, Mjåset has shifted his worldview about the latter category of care. Researchers, he says, suggest that “3 out of 10 times your doctor prescribes or suggests something that is completely unnecessary. You know what they claim the reason for this is? Patient pressure.”
For many of us, the whole process of receiving healthcare — making an appointment, waiting for it to arrive, rearranging our schedule so we can go, showing up for it — takes considerable time and energy. We may feel, consciously or not, that our efforts need to yield a concrete result. We want to leave our encounter with a doctor bearing a diagnosis, plan of action, prescription, or some other decisive, active response.
Mjåset believes that both physicians and patients need to be vigilant about excessive care. He says, “A good doctor sometimes says no, but the sensible patient also sometimes turns down an opportunity to get diagnosed or treated.” When he spoke to his colleagues about his patient and her question, they said they’d also never been asked: “Is it necessary?”
He suggests 4 questions that we should pose to our doctors the next time they recommend a medication, procedure, test, treatment or surgery.
Is this really necessary?
What are the risks?
Are there other options?
What happens if I don’t do anything?
Mjåset knows raising these questions is easier said than done. It’s especially true given the limited time most people have with healthcare providers. In a 2017 study, doctors’ appointments in the 18 countries that accounted for half the world’s population lasted for five minutes or less; even countries like Sweden and the US had average appointment lengths of 22 minutes and 20 minutes, respectively. But he urges us to speak up. He says, “You need to get in the front seat with your doctor and start sharing decisions on where to go.”
Asking these 4 questions, he says, will help us and our doctors. They can reduce the burden and cost of unnecessary care on our overall system and prevent us from suffering complications and side effects that could have been avoided. As he puts it, “People like me need your help.”
Watch his TEDxOslo talk here:
Daryl Chen is the Ideas Editor at TED.
Jul 31, 2019 / Amanda Little

The summer of 2019 has seen heat records tumble like dominoes across the Northern Hemisphere. On May 26, the thermometer climbed to 102 in Savannah, Georgia, an all-time high for that month; the same day, it hit an unprecedented 103.1 in Hokkaido, Japan’s northernmost island. Then, in June, a three-week heat wave tore through Pakistan and India, where it reached 123.4 in the central city of Churu. In July, it was Western Europe’s turn when the temperature soared to 108.7 in Paris and 102.2 in Brussels.
Of course, intense heat doesn’t occur in a vacuum. It’s accompanied by water shortages and drought, which are expected to be the new norm on our planet. In the US, drought has become associated with California. In fact, from December 20, 2011, through March 5, 2019, some form of drought existed somewhere in the state. This prolonged parching has resulted in billions of dollars in agricultural losses and the death of over 100 million trees in state forests alone.
Below, journalist Amanda Little goes to Southern California to learn more about two sources of drinking water which the state — and our planet — will be tapping in coming years.
Almost all of the water consumed by the 22 million people of California’s water-stressed southern region is imported. Much of it is pumped long distances, over mountains, from Northern California. Southern California also draws heavily from the Colorado River, the beleaguered waterway that supplies six other states and Mexico. As these freshwater sources have dwindled, the cost of water imported to Southern Californian cities has been climbing nearly 10 percent a year. The changing economics of water have forced utilities to turn in a new direction for relief: westward to the Pacific Ocean.
California has 840 miles of coastline adjoining the world’s largest ocean, an oversupply of brine lapping up against an increasingly thirsty landscape. In order to tap this massive reservoir, the San Diego Water Authority partnered with the Israeli company IDE to build a $1 billion desalination plant in Carlsbad, a suburb of San Diego. It opened in 2017, the largest desalination facility in the Western Hemisphere.
“If we could ever competitively, at a cheap rate, get freshwater from salt water, that … would really dwarf any other scientific accomplishments,” President John F. Kennedy told the Washington press corps in the 1960s.
Mark Lambert, the head of IDE’s U.S. division, who oversaw the building of the Carlsbad plant, describes desalination as “the most significant kind of modern alchemy. About 97 percent of the earth’s water is in the ocean, yet only recently have we been able to tap that resource to grow crops or quench human thirst.”
“Desalination may seem like a panacea, but from a cost and energy standpoint it’s the worst deal out there,” says Sara Aminzadeh of the California Coastkeeper Alliance.
Desalination has been around for millennia if you count the evaporation techniques pioneered by the ancient Greek. Sailors in the 4th century BC boiled salt water and then captured the steam. When cooled, steam condenses into distilled water that’s free of virtually all contaminants. This same basic technology — thermal desalination — is still used in places like Saudi Arabia, where fuel for boiling the water comes cheap. Since the 1960s, most desalination operations use reverse osmosis (RO), a method that simulates the biological process that happens within our cells as fluids flow across semipermeable membranes.
There remain big challenges for desalination, and number one is the energy cost. A NASCAR vehicle does about 700 horsepower at full throttle. By contrast, the series of pumps at the Sorek plant near Tel Aviv — the world’s largest desalination facility, which processes some 200 million gallons daily — collectively exert roughly 7000 horsepower of energy (or 1100 pounds per square inch of pressure) night and day.
Improvements in the pumps, pipe design and membranes have cut the total amount of energy used in desalination by about half in the past two decades. The energy demands will come down further as efficiencies improve, but many see it as a sticking point.
Sara Aminzadeh, the executive director of the California Coastkeeper Alliance, one of many environmental groups that have opposed the development of desalination plants in California, tells me, “Desalination may seem like a panacea, but from a cost and energy standpoint it’s the worst deal out there.”
The Carlsbad deslination plant provides nearly 1/10th of San Diego County’s total water supply — enough for about 400,000 county residents.Up the coast, another large desalination plant is under construction in Huntington Beach, which will supply drinking water to LA suburbs. More than a dozen similar plants have been proposed along California’s southern and northern coastlines.
Daily, the Orange County plant pumps out 100 million gallons of drinking water. The sewage moves through eight stages of filtration before it is drinkable.
But there’s another source that’s becoming even more critical to the future water supply, one that officials call “recycled wastewater,” a pleasant term for human sewage. This is one of the harder realities I’ve come to accept about modern agriculture — that everything we’re now flushing down our toilets and pouring down our drains may have to play an important role in feeding us and growing our food.
“We call it the big tooth comb — step one of the filtration process!” Snehal Desai, Global Business Director of Dow Water & Process Solutions, shouts above the sound of sluicing water. There’s a visible torrent of raw sewage water flowing through a channel below us at the Orange County Sanitation District, a facility that treats waste from the toilets, showers, sinks and gutters of 1.5 million suburban Californians. An enormous rake descends into the depths of the sewage flow and brings up cardboard, wet wipes, tampons, egg shells, marbles, toys, tennis balls, sneakers — all the detritus that can’t fit through the screen covering the plant’s intake.
The flow that passes through the screen has begun a journey through an advanced purification process that culminates in a stage of RO filtration. Daily, the plant pumps out 100 million gallons of drinking water — enough to supply 850,000 county residents — which makes this the largest “toilet-to-tap” facility on the planet. The sewage moves through eight stages of filtration, including a gravel-sand filter and a bacterial “bioscrubbing” process used in Israeli plants. Orange County also has a “microfiltration” stage, in which the water is sucked through thousands of tiny porous straws. In the final and most critical stage, the water is forced through a massive hive of cylinders containing the RO membranes.
This Orange County facility is setting a precedent for the use of sewage to produce drinking water every bit as pure as the water that comes from desalination. This process is cheap compared to desalination — about half the cost. Sewage has much lower salinity than seawater, which makes it easier to process. “Recycled wastewater is the fastest-growing area in the water industry. Why? Because not every city has an ocean, not everyone has good lakes and rivers, but everybody’s got sewage,” says Desai. “That’s the megatrend.”
“Accepting recycled wastewater is kind of like being asked to wear Hitler’s sweater,” says social psychologist Paul Rozin.
San Diego recently announced plans to produce 35 percent of its water from recycled sewage by 2030 — not just for irrigation but for drinking. It has completed designs on a toilet-to-tap facility larger than Orange County’s. Still, there are barriers to overcome, and the gross factor is first among them. Even the desperation of drought can’t eliminate the fact that drinking your own waste is nobody’s first choice, unless you’re a resident of the international space station.
“Accepting recycled wastewater is kind of like being asked to wear Hitler’s sweater,” says Paul Rozin, a social psychologist at the University of Pennsylvania who has consulted water utilities on marketing toilet-to-tap programs to residents. “No matter how many times you clean the sweater, you just can’t take the Hitler out of it.”
But the purity you get from the RO process is quantifiably better than the water you get from conventional treatments — better even than some bottled water. “What flows from our membranes is the Rolls-Royce of municipal water,” says Desai. Whereas tap water is often treated with chemical coagulants and chlorine, RO filtration is a mechanical filtration of water contaminants that cuts the need for those chemicals. It’s analogous to the mechanical removal of weeds in a field practiced by organic farmers in lieu of chemical pesticides: “Think of it as ‘organic’ tap water,” says Desai.
For now, Dow is focused on making membrane products for big industrial and municipal water systems, but it envisions micro-scale systems down the line. Bill Gates made a pitch for a similar approach when he blogged a few years back about watching a pile of human feces on a conveyor belt enter a small-scale waste-treatment plant built to serve a community of a few thousand people in Senegal, and, in minutes, get converted into “water as good as any I’ve had out of a bottle. I would happily drink it every day.”
Desai predicts that water filtration technology will become decentralized everywhere. We’ll control and regenerate our own water supplies farm by farm, neighborhood by neighborhood, or household by household. Eventually the water production could become, like the food production, circular — a closed-loop system in which 100 percent of water that goes down commercial and residential drains is recycled; whatever is lost in evaporation or leakage can be made up for with desalinated salt water that moves through shared networks. Although the vision is at least decades from becoming a reality, it may be necessary to our future food security and critical to our survival.
At the end of my tour of the Orange County plants, we arrive at a shining stainless-steel sink where water that hours earlier had begun as raw sewage was now flowing crystal clear from the tap. Desai filled up two Dixie cups. “To the future!” he toasted. I shuddered as I knocked mine back. But somehow, the stuff tasted every bit as good as water that had bubbled up from a spring in the Alps. I poured myself a second cup.
Excerpted with permission from the new book The Fate of Food: What We’ll Eat in a Bigger, Hotter, Smarter World by Amanda Little. Published by Harmony Books, an imprint of the Crown Publishing Group, a division of Penguin Random House LLC. Copyright © 2019 Amanda Little.
Watch her TEDxNashville talk now:
Amanda Little is a professor of journalism and writer-in-residence at Vanderbilt University. Her reporting on energy, technology and the environment has taken her to ultra-deep oil rigs, down manholes, and inside monsoon clouds. Little’s work has appeared in publications ranging from The New York Times and The Washington Post to Wired, Rolling Stone and Bloomberg Businessweek. She is also the author of the book Power Trip: From Oil Wells to Solar Cells — Our Ride to the Renewable Future.

Your Friday prompt for Stream of Consciousness Saturday is “astronomical.” Use it any way you like. Have fun!
There are so many ways I could use astronomical, gas prices, trade tariffs, my dogs constant desire for attention but the weather seems more appropriate. Many do not believe in Global Warming, they don’t see the ancient ice melting or water levels rising but it’s hard to argue with global temperatures. Europe is sweltering, the news has shown people cooling off in the fountains. Here in America it’s a major heat warning for half of the US with record breaking temps. I even let my flowers die because I would not go out in the astronomical heat.
That might not be a proper way to use the word, or a cheesy way out but today that’s all there is. Have a great weekend. M

Here are the rules for SoCS:

My Parathyroid surgery was July 8th and I’m healing nicely. The surgeon found quite a surprise, I had five Parathyroids instead of four. She said it was rare. I hope that translates to feeling all the better. She is getting my calcium levels adjusted and it was painful in the beginning with cramping legs and numb fingers.
It’s not what you take, it’s what you leave at home! Hospital don’t have to make all of your medicines available to you when you stay over. Either check with the hospital to see what on your list is not available or guess that the most expensive and newest ones won’t be available. That’s a crap shoot but it has worked.
I didn’t plan on staying in the hospital so I didn’t give any consideration to what meds I needed, boy was that a mistake. They didn’t have three of the meds I’m addicted to and it set off a mini withdrawal for two days.
Thank you for reading, your a good friend and I appreciate you. Have a great day. Drink plenty of water and get in the a/c or shade often to avoid overheating.
Melinda


WEB MD
By Stephanie Hairston
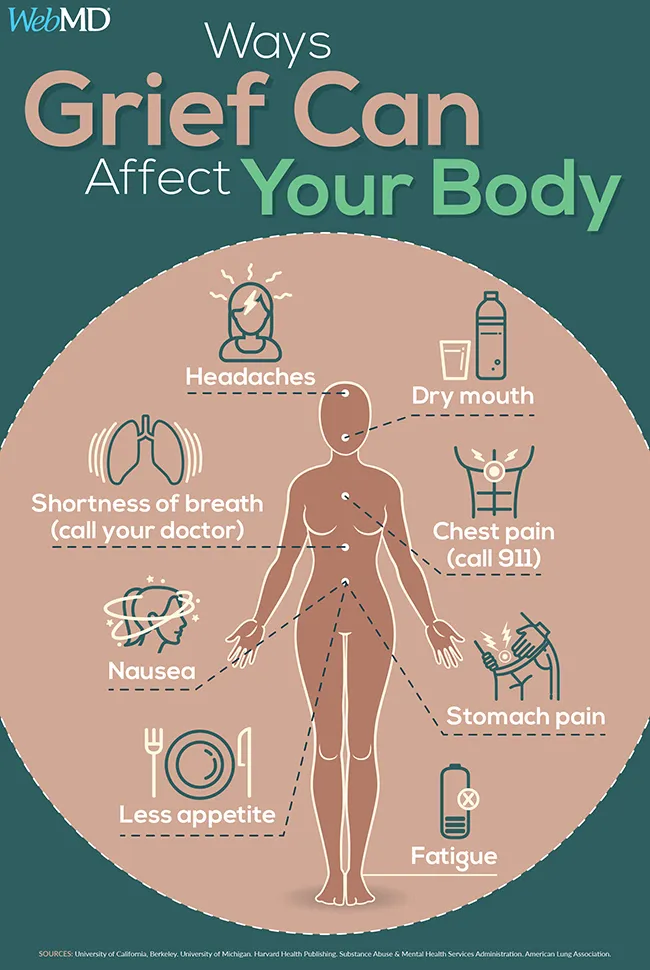
July 11, 2019 — It’s surprising how physical grief can be. Your heart literally aches. A memory comes up that causes your stomach to clench or a chill to run down your spine. Some nights, your mind races, and your heart races along with it, your body so electrified with energy that you can barely sleep. Other nights, you’re so tired that you fall asleep right away. You wake up the next morning still feeling exhausted and spend most of the day in bed.

Amy Davis, a 32-year-old from Bristol, TN, became sick with grief after losing Molly, a close 38-year-old family member, to cancer. “Early grief was intensely physical for me,” Davis says. “After the shock and adrenaline of the first weeks wore off, I went through a couple of months of extreme fatigue, with nausea, headaches, food aversion, mixed-up sleep cycles, dizziness, and sun sensitivity. It was extremely difficult to do anything. … If there’s one thing I want people to know about grief, it’s how awful it can make your body feel.”
What causes these physical symptoms? A range of studies reveal the powerful effects grief can have on the body. Grief increases inflammation, which can worsen health problems you already have and cause new ones. It batters the immune system, leaving you depleted and vulnerable to infection. The heartbreak of grief can increase blood pressure and the risk of blood clots. Intense grief can alter the heart muscle so much that it causes “broken heart syndrome,” a form of heart disease with the same symptoms as a heart attack.
Stress links the emotional and physical aspects of grief. The systems in the body that process physical and emotional stress overlap, and emotional stress can activate the nervous system as easily as physical threats can. When stress becomes chronic, increased adrenaline and blood pressure can contribute to chronic medical conditions.
Research shows that emotional pain activates the same regions of the brain as physical pain. This may be why painkilling drugs ranging from opioids to Tylenolhave been shown to ease emotional pain.
Depression is not a normal part of grief, but a complication of it. Depression raises the risk of grief-related health complications and often requires treatment to resolve, so it’s important to know how to recognize its symptoms. Sidney Zisook, MD, a grief researcher and professor of psychiatry at the University of California, San Diego, says people can distinguish normal grief from depression by looking for specific emotional patterns.
“In normal grief, the sad thoughts and feelings typically occur in waves or bursts followed by periods of respite, as opposed to the more persistent low mood and agony of major depressive disorder,” Zisook says.
He says people usually retain “self-esteem, a sense of humor, and the capacity to be consoled or distracted from the pain” in normal grief, while people who are depressed struggle with feelings of guilt and worthlessness and a limited ability “to experience or anticipate any pleasure or joy.”
Complicated grief differs from both depression and normal grief. M. Katherine Shear, MD, a professor of psychiatry at Columbia University’s School of Social Work and director of its Center for Complicated Grief, defines complicated grief as “a form of persistent, pervasive grief” that does not get better naturally. It happens when “some of the natural thoughts, feelings, or behaviors that occur during acute grief gain a foothold and interfere with the ability to accept the reality of the loss.”
Symptoms of complicated grief include persistent efforts to ignore the grief and deny or “rewrite” what happened. Complicated grief increases the risk of physical and mental health problems like depression, anxiety, sleep issues, suicidal thoughts and behaviors, and physical illness.
Margaret Stroebe, PhD, a bereavement researcher and professor of clinical psychology at Utrecht University, says that recent research has shed light on many of “the cognitive and emotional processes underlying complications in grieving, particularly rumination.”
Research shows that rumination, or repetitive, negative, self-focused thought, is actually a way to avoid problems. People who ruminate shift attention away from painful truths by focusing on negative material that is less threatening than the truths they want to avoid. This pattern of thinking is strongly associated with depression.
Rumination and other forms of avoidance demand energy and block the natural abilities of the body and mind to integrate new realities and heal. Research by Stroebe, and others shows that avoidance behavior makes depression, complicated grief, and the physical health problems that go with them more likely. Efforts to avoid the reality of loss can cause fatigue, weaken your immune system, increase inflammation, and prolong other ailments.
When someone close to you dies, your social role changes, too. This can affect your sense of meaning and sense of self.
Before losing Molly, Davis says she found a personal sense of value in “being good at helping other people and taking care of them.” But after Molly died, she felt like she “couldn’t help anyone for a while.” Losing this role “dumped the bucket” of her identity “upside down.” Davis says, “I felt like I had nothing to offer. So I had to learn my value from other angles.”
Caregivers face especially complicated role adjustments. The physical and emotional demands of caregiving can leave them feeling depleted even before a loved one dies, and losing the person they took care of can leave them with a lost sense of purpose.
“Research shows that during intense caregiving periods, caregivers not only experience high levels of stress, they also cannot find the time and energy to look after their own health,” says Kathrin Boerner, PhD, a bereavement researcher and professor of gerontology at the University of Massachusetts in Boston.
“This can result in the emergence of new or the reemergence of existing ‘dormant’ health problems after the death of the care recipient. These health issues may or may not be directly related to the caregiver’s grief experience, but they are likely related to the life situation that was created through the demands of caregiving,” Boerner says.
It can be hard to make life work again after a close family member dies. Losing a partner can mean having to move out of a shared home or having to reach out to other loved ones for help, which can further increase emotional stress and worry. Strobe says the stress of adjusting to changes in life and health during and after a loss can “increase vulnerability and reduce adaptive reserves for coping with bereavement.”
Emotional and physical self-care are essential ways to ease complications of grief and boost recovery. Exercising, spending time in nature, getting enough sleep, and talking to loved ones can help with physical and mental health.
“Most often, normal grief does not require professional intervention,” says Zisook. “Grief is a natural, instinctive response to loss, adaptation occurs naturally, and healing is the natural outcome,” especially with “time and the support of loved ones and friends.”
For many people going through a hard time, reaching out is impossible. If your friend is in grief, reach out to them.Amy Davis
Grief researchers emphasize that social support, self-acceptance, and good self-care usually help people get through normal grief. (Shear encourages people to “plan small rewarding activities and try to enjoy them as much as possible.”) But the researchers say people need professional help to heal from complicated grief and depression.
Davis says therapy and physical activities like going for walks helped her cope. Social support helped most when friends tried to reach out instead of waiting or asking her to reach out to them.
“Th thing about grief and depression and sorrow and being suicidal is that you can’t reach out. For many people going through a hard time, reaching out is impossible. If your friend is in grief, reach out to them. Do the legwork. They’re too exhausted!”
Davis’ advice to most people who are grieving is to “Lean into it. You only get to grieve your loved one once. Don’t spend the whole time trying to distract yourself or push it down. It does go away eventually, and you will miss feeling that connected to that person again. And if you feel like your whole life has fallen apart, that’s fine! It totally has. Now you get to decide how to put yourself back together. Be creative. There’s new life to be lived all around you.
“WebMD News Special Report Reviewed by Neha Pathak, MD on July 11, 2019


